Among the many untoward effects of diabetes on the body is a potential impact on oral health, specifically a high risk of periodontal disease. Is there anything in its disease course that eyecare providers should be alerted to, given the obvious importance of screening for diabetic retinopathy (DR)? To help understand comorbid diabetes-related complications, authors of a recent systemic review and meta-analysis aimed to investigate the association between DR and periodontitis in patients with type 1 and type 2 diabetes. While they did find an association between the two—possibly due to shared inflammation pathways—the overall certainty of evidence is low.
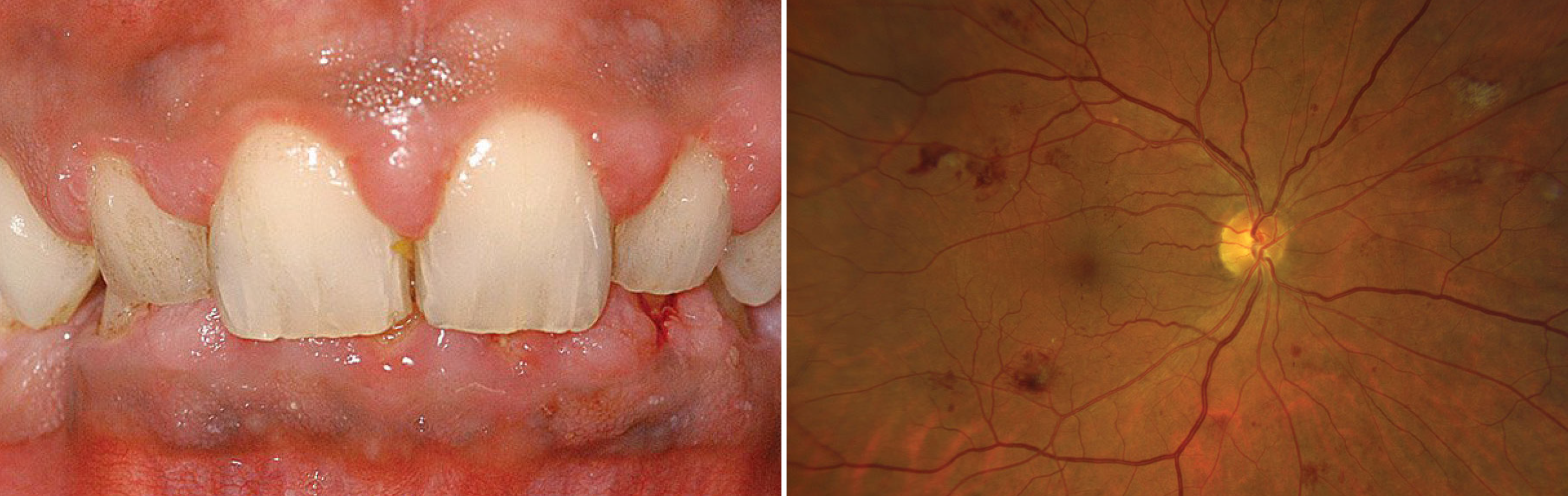 |
| Shared inflammation pathways may explain the link between periodontitis and DR, but further research is needed to determine how strong the connection is or if this applies to all diabetic patients. Photo: BPI Dental; Jay Haynie, OD. Click image to enlarge. |
Ten studies on the association between DR and periodontitis were evaluated, eight of which found a significant association. Meta-analysis of 843 participants showed diabetic patients with periodontitis had about 4.5 times higher odds of developing DR.
However, an analysis indicated very low certainty of evidence. That, combined with the high heterogeneity among the included studies complicates the reliability of these conclusions, highlighting the need for a cautious interpretation, the authors noted in their paper on the work for International Dental Journal.
“When we removed studies with a high risk of bias, we found that the link between periodontitis and retinopathy in diabetic patients became less clear,” the researchers wrote, explaining that the connection was no longer statistically significant. “This means that when we only looked at the most reliable studies, we couldn’t be as confident that there’s a strong link between periodontitis and retinopathy in diabetes.”
These findings highlight not just the need for a cautious interpretation, but why more high-quality research is needed. While the results suggest a connection between periodontitis and DR, “we can’t say how strong this connection is or if it applies to all diabetic patients,” they wrote.
Shared inflammation pathways may explain the link between periodontitis and DR. Both conditions are characterized by elevated levels of inflammatory mediators such as IL-1b, IL-6, TNF-a and CRP, which can promote endothelial damage and exacerbate diabetes-associated vascular pathology, potentially contributing to the development of DR.
“Furthermore, the systemic inflammation associated with periodontitis may trigger atherosclerosis and retinal hypoxia, promoting retinal neovascularization,” the article explains. “Elevated inflammatory markers can also drive adipose tissue inflammation, causing dyslipidemia and ectopic fat accumulation in the endothelium, further contributing to DR progression.”
While current evidence does not support definitive clinical recommendations, it underscores the importance of comprehensive care for diabetic patients, including oral and ocular health monitoring. The authors suggest that while providers should be aware of this possible link, they should base clinical decisions on individual patient factors.
| Click here for journal source. |
Anil S, Joseph B, Anjali Pereira M, et al. Diabetic retinopathy and periodontitis: implications from a systemic review and meta-analysis. International Dental Journal. October 27, 2024. [Epub ahead of print.] |


