 |
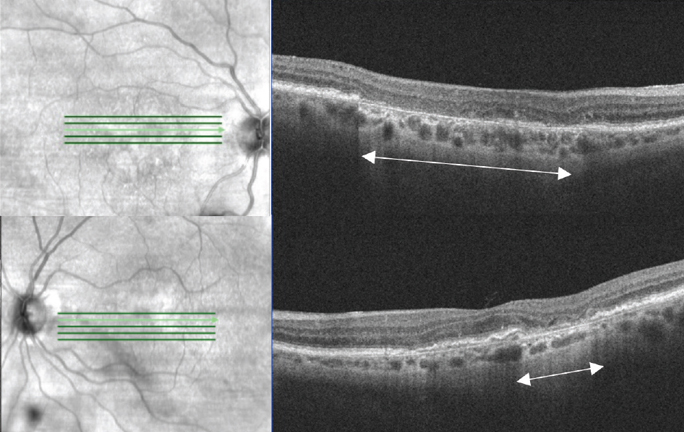
| Some outcomes, including key endpoints of microperimetry average threshold and atrophic lesion size, indicate that PPS toxicity in many cases may be a relentlessly progressive degenerative maculopathy. These findings should inform PPS prescribing patterns, patient counseling and disease monitoring strategies. One key feature to look for is cRORA (seen here in a GA patient). Photo: Anna Bedwell, OD. Click image to enlarge. |
The maculopathy associated with chronic pentosane polysulfate (PPS) use can pose serious risk to vision and, alarmingly, continues to progress even after drug cessation. Authors of a recent study reported on this and found that functional and structural outcomes continue to deteriorate even several years after stopping PPS. The team’s paper on the work was recently published in American Journal of Ophthalmology.
A total of 23 eyes of 12 participants (11 of them women) diagnosed with PPS maculopathy were included; median age was 58. Participants were followed for four years. Changes in visual function and structure were the primary outcomes measured. Patient-reported outcomes were assessed with the Visual Function Questionnaire (VFQ-39) and the Low Luminance Questionnaire (LLQ). Structural outcomes included the presence of complete RPE and outer retinal atrophy (cRORA), atrophic lesion size (in mm2), macular central subfield thickness and subfoveal choroidal thickness.
The findings of this study suggest that PPS maculopathy continues to progress many years after drug cessation, with broad-ranging and disabling impacts on retinal structure and visual function. The majority of eyes exhibited macular cRORA by the final visit, with some developing new onset atrophy years after PPS cessation.
All participants exhibited retinal function and structure decline between the baseline and four-year visit. The VFQ-39 composite scores at four years (52, range 44-60) were lower than previously reported in patients with geographic atrophy (61.7 ±16.3) and diabetic macular edema (65.0 ±19.7). On subscale analysis, the greatest declines occurred in the ‘dependency’ and ‘role difficulties’ subscales. LLQ composite scores at four years were significantly lower than those reported in patients with intermediate and advanced AMD, with the greatest declines occurring in the ‘emotional distress’ and ‘extreme lighting condition’ subscales.
All eyes with cRORA at baseline demonstrated lesion growth. The median growth rate of atrophic lesions (0.23mm/year) was lower than, yet comparable to, others reported in previous studies (0.32mm/year and 0.26mm/year). The median growth rate did not significantly differ from the rate seen at the two-year visit (0.23mm/year). For context, a meta-analysis reported the mean growth rate for geographic atrophy in patients with AMD to be 0.33mm/year (SD, 0.17mm/year).
Additionally, five eyes developed new-onset cRORA during the study period, with one participant developing it eight years after stopping PPS at the age of 49. It should be noted that the development of cRORA years after PPS cessation has been found in prior studies as well.
Disease progression following drug cessation is not unsurprising, as similar findings have been observed in other toxic maculopathies, most notably hydroxychloroquine toxicity, the authors noted in their paper on the research. Additionally, many other diseases demonstrate that once present, cRORA lesions tend to grow.
The authors concluded that regardless of mechanism, this finding of new-onset atrophy years after drug cessation is “alarming” and should be investigated further. “For instance, to better guide screening programs and prognostication, it would be helpful to identify early signs of toxicity at which patients do not ultimately progress to atrophy if PPS use is halted,” they wrote. “Additionally, with these findings of continued atrophy progression, it may be worthwhile to investigate the potential role of existing therapies that may slow the progression of geographic atrophy in age-related macular degeneration, including Age-Related Eye Disease Study antioxidants, complement inhibitors and photobiomodulation.”
| Click here for journal source. |
Hall BP, Shiromani S, Jung EH, et al. Pentosan polysulfate maculopathy: final outcomes from a four-year prospective study of disease progression after drug cessation. Amer J Ophthalmol. December 3, 2024. [Epub ahead of print.] |


