While ocular complications are well-known with preterm births, it has been suggested that retinal structural vascular abnormalities can persist for years. This is thought in cases of severe retinopathy of prematurity (ROP) and is suspected due to the treatment received. Consequently, researchers wanted to look at the macular microvasculature condition of ROP cases who were treated with intravitreal bevacizumab compared with preterm births without ROP and spontaneously regressed ROPs.
 |
|
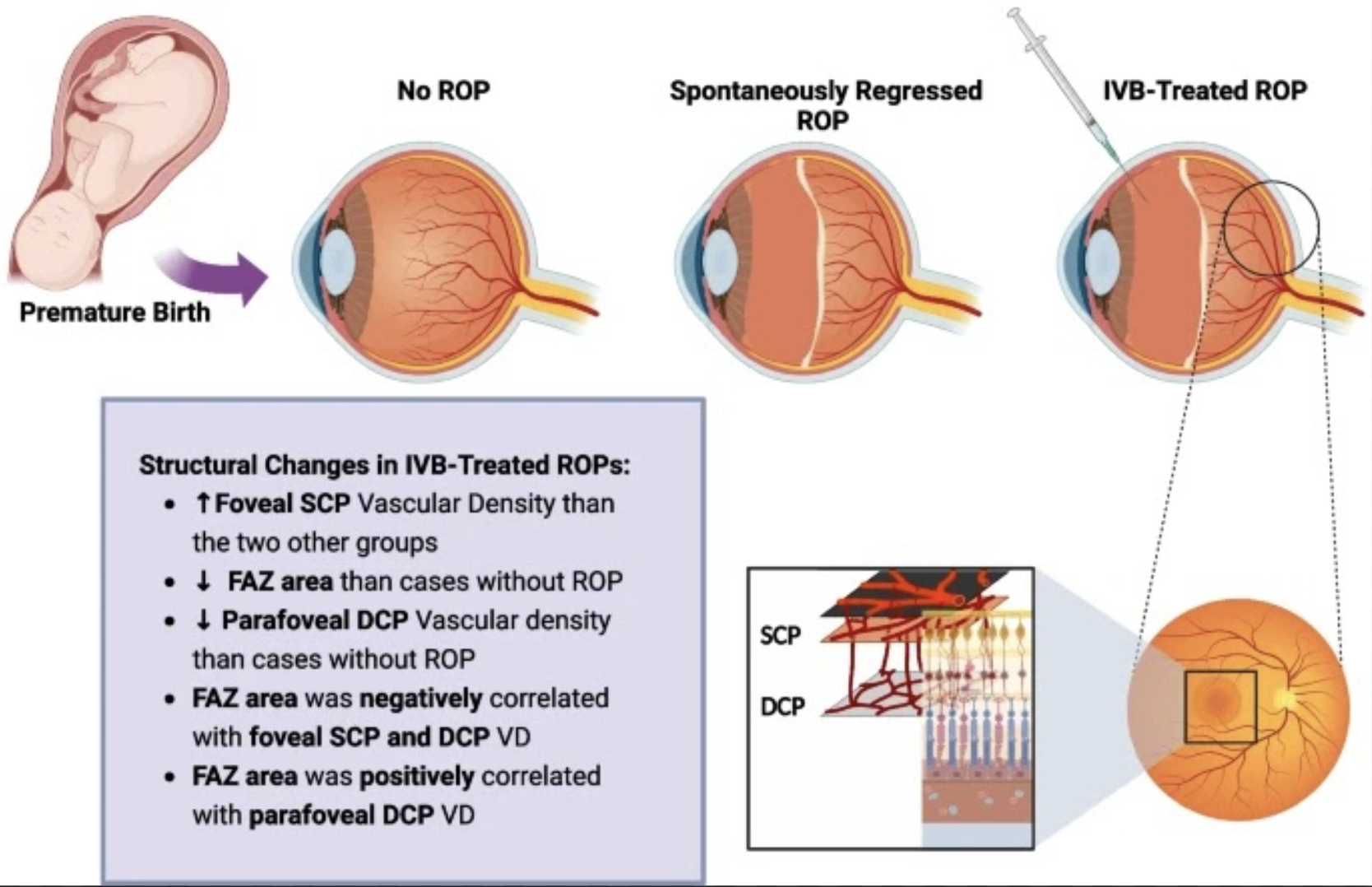
One possible reason for differences in the foveal avascular zone could be due to related ischemia induced by lower parafoveal deep plexus vascular density, leading to pigment epithelial-derived factor and increased VEGF in the foveal region. This would induce greater development and migration of vessels the center of the macula. Photo: Milani AE, et al. BMC Ophthalmol. 2024;24:505. Click image to enlarge. |
The retrospective investigation included 50 premature neonates who were classified into three groups: preterm cases without ROP, spontaneously regressed ROPs and bevacizumab-treated ROPs. All who were part of the study were evenly split by sex, with 25 girls and 25 boys, with a median age of five. Of all 50 kids, 26 eyes evaluated fell into the category of having no ROP, 50 belonged to the spontaneously regressed ROP group and 24 to the bevacizumab group.
The group of spontaneously regressed cases involved 25 zone-2 and 25 zone-3 ROPs, while the treatment group had nine zone-1 and 15 zone-2 ROPs. Zone-2 cases were also found to be more advanced in the IBV group, as well as treated eyes showing a higher foveal superficial capillary plexus vascular density (28.5%) vs. the no ROP group (23.1%) and spontaneous group (22.9%). Conversely, the parafoveal deep capillary vascular density was lower in treated eyes (48.5%) than in eyes without ROP (53.4%). Another difference that was observed was the foveal avascular zone being smaller in treated eyes (0.11mm2) vs. non-ROP eyes (0.22mm2). The area of the foveal avascular zone was positively correlated with the foveal superficial and deep capillary plexus’ vascular density and negatively correlated with parafoveal deep plexus vascular density.
Upon discussion, the authors of the study write how microvascular abnormality presence was significantly higher in the IBV group than the spontaneous group. They explain that this mainly was due to more advanced cases existing in the bevacizumab group. Also, based on their findings, microvascular abnormalities were linked with more advanced ROPs and worse best-corrected visual acuity.
The authors report two potential mechanisms for the differences seen in the foveal avascular zone. One has to do with the role of pigment epithelial-derived factor in this area development and its relationship to pan-retinal photocoagulation and anti-VEGF factors.
More generally, the authors believe their findings suggest that although ROP and its treatment with intravitreal bevacizumab “may have an excellent functional outcome, it may have some unknown structural impacts on the macular development.”
| Click here for journal source. |
Milani AE, Ahoor MH, Etemad F, Ghadim BK, Arasteh A. The macular microvascular changes in children with a history of retinopathy of prematurity treated with intravitreal Bevacizumab injection using optical coherence tomography: a retrospective cohort. BMC Ophthalmol. 2024;24:505. |



